Returning to Sports & Fitness Activities Following COVID-19
In the current climate of public health in the US, we must consider the implications of COVID-19 for nearly every activity. We have learned to modify how we socialize, exercise, and participate in our usual activities. Nearly a year into the pandemic, many of us have resumed playing sports. This is beneficial on many levels for youth athletes, but there is no denying that participation in any group activity comes with a risk of being infected with the COVID-19 virus. While there are many protocols in place to mitigate this risk, there are still cases that arise among athletes.
In addition to the many possible symptoms of the virus, there are often underlying effects of the virus that may go unrecognized. Patients with COVID-19 are found to be 22% more likely to develop some form of heart damage compared to other infectious diseases. One of the most common forms of cardiovascular complications is myocarditis, which has been found at an alarming rate in athletes in the months following a COVID-19 diagnosis. Myocarditis is an inflammation/infection of the heart, which can compromise the heart’s ability to pump blood to the rest of the body and place increased stress on the heart. Another study found that only 1.4% of 145 student athletes diagnosed with COVID-19 had myocarditis after a cardiac MRI. This is likely to vary, and the sample size is relatively small compared to the number of positive cases.
Recently, Keyontae Johnson, star basketball player of the Florida University Gators, collapsed on the court. The cause of his collapse was determined to be myocarditis, just a few months after being diagnosed with COVID-19. While he is recovering well, this could have easily resulted in a worse outcome. There are many severe and potentially deadly outcomes that can result from myocarditis if not treated properly, which is why it is extremely important that an athlete follow an appropriate return-to-play progression following a COVID-19 diagnosis. This allows the heart to progressively recover and adapt to the demands of exercise and sport.
So what exactly does a gradual return to play progression look like? It consists of multiple steps that are progressed only after the athlete has met specific criteria. It is important to consider that an athlete should have at least 10 days of rest, discontinued all treatment/medication for the virus, and be symptom-free for 7 days before even beginning the progression. They should also be able to walk at least 500 meters and be able to perform all activities of daily living without any breathlessness or excessive fatigue. This should also be considered for the general public before returning to the gym and exercise! A study in the British Journal of Sports Medicine recently published a return to play progression that allows safe return to sport via gradual progressions and monitoring of the athlete’s response. When at all possible, it is extremely valuable to monitor heart rate, rating of perceived exertion, oxygen saturation, and overall perception of fatigue. It is important to note that research surrounding the virus is still in its infancy, meaning that things and information will likely change frequently.
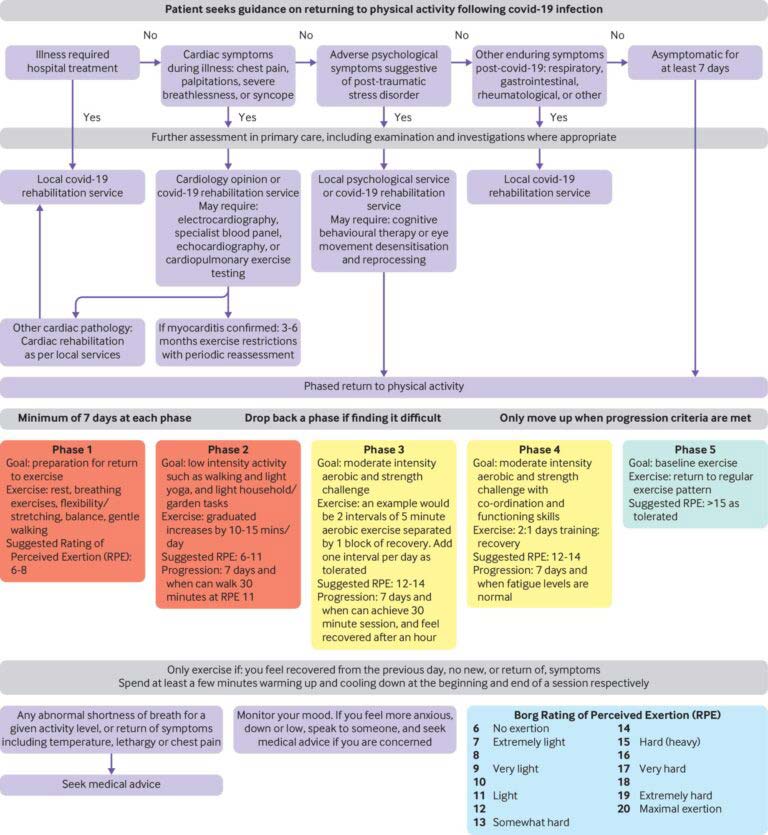
Below you will find an example of a return-to-play progression published by the BJSM and a return-to-activity flow sheet based on severity of illness to help guide you through the process. If you or an athlete in your family has questions about returning to sports following a COVID-19 infection and illness, please consult your physician. In addition, the physical therapists, athletic trainers, and training staff here at Elite Sports Performance & Physical Therapy in Stoughton and Foxboro can help guide you through these stages and back to a safe return to sport.

References
Elliott N, Martin R, Heron N, et alInfographic. Graduated return to play guidance following COVID-19 infection. British Journal of Sports Medicine 2020;54:1174-1175.
Barati A, Naderifar H. Return to Sports Activities in athletes with Covid-19 with a Cardiovascular Approach. Journal of Shahid Sadoughi University of Medical Sciences. 2020. doi:10.18502/ssu.v28i10.4918
